Abstract
Aims/hypothesis
Treatment with glucocorticoids, especially at high doses, induces insulin resistance. The aims of the present study were to identify the potential defects in insulin signalling that contribute to dexamethasone-induced insulin resistance in skeletal muscles, and to investigate whether the glycogen synthase-3 (GSK-3) inhibitor CHIR-637 could restore insulin-stimulated glucose metabolism.
Materials and methods
Skeletal muscles were made insulin-resistant by treating male Wistar rats with dexamethasone, a glucocorticoid analogue, for 12 days. Insulin-stimulated glucose uptake, glycogen synthesis and insulin signalling were studied in skeletal muscles in vitro.
Results
Dexamethasone treatment decreased the ability of insulin to stimulate glucose uptake, glycogen synthesis and glycogen synthase fractional activity. In addition, the dephosphorylation of glycogen synthase by insulin was blocked. These defects were paralleled by reduced insulin-stimulated protein kinase B (PKB) and GSK-3 phosphorylation. While expression of PKB, GSK-3 and glycogen synthase was not reduced by dexamethasone treatment, expression of the p85α subunit of phosphatidylinositol 3-kinase (PI 3-kinase) was increased. Inhibition of GSK-3 by CHIR-637 increased glycogen synthase fractional activity in soleus muscle from normal and dexamethasone-treated rats, although the effect was more pronounced in control rats. CHIR-637 did not improve insulin-stimulated glucose uptake in muscles from dexamethasone-treated rats.
Conclusions/interpretation
We demonstrated that chronic dexamethasone treatment impairs insulin-stimulated PKB and GSK-3 phosphorylation, which may contribute to insulin resistance in skeletal muscles. Acute pharmacological inhibition of GSK-3 activated glycogen synthase in muscles from dexamethasone-treated rats, but GSK-3 inhibition did not restore insulin-stimulated glucose uptake.
Similar content being viewed by others
Introduction
Glucocorticoids in excess induce insulin resistance. This has been documented in patients with Cushing’s syndrome [1], during glucocorticoid treatment [2], in glucocorticoid clinical trials [3], and in conjunction with mental stress [4]. It has even been suggested that high-fat diets cause insulin resistance via increased glucocorticoid production [5]. The receptors for glucocorticoids belong to the nuclear receptor family [6]. When a glucocorticoid binds to its receptor, the receptor translocates to the nucleus, where it binds to glucocorticoid response elements on DNA and regulates transcription of specific genes [7].
Insulin enhances glucose transport by stimulation of GLUT4 translocation from intracellular vesicles to the cell membrane [8]. When insulin binds to its receptor, the latter becomes tyrosine-phosphorylated and activates IRS-1. Tyrosine-phosphorylated IRS-1 binds the p85α regulatory subunit of phosphatidylinositol 3-kinase (PI 3-kinase) and the p110 catalytic subunit becomes activated [9]. Protein kinase B (PKB) is subsequently activated by phosphorylation at Thr308 and Ser473 [9]. Once activated, PKB phosphorylates glycogen synthase kinase-3 (GSK) (GSK-3α at Ser21, GSK-3β at Ser9), deactivating the kinase [10]. GSK-3 inactivation promotes glycogen synthase activation and increases glycogen synthesis [11]. Moreover, PKB mediates insulin-stimulated GLUT4 translocation [12, 13], but the complete signalling pathway remains unknown.
Skeletal muscles represent the predominant peripheral site of insulin-dependent glucose disposal [14]. Adequate regulation of blood glucose requires that excess glucose is incorporated into skeletal muscle glycogen [15], and insulin resistance in skeletal muscles plays a key role in the development of type 2 diabetes. Chronic treatment with the glucocorticoid analogue dexamethasone decreases insulin-stimulated glucose uptake and GLUT4 translocation in skeletal muscle without reducing the total content of GLUT4 [16, 17]. Dexamethasone treatment, in addition, inhibits insulin-stimulated glycogen synthesis and glycogen synthase activation [18, 19].
Many investigations have focused on identifying the insulin signalling steps that are impaired in insulin-resistant muscles and a number of studies have reported reduced activation of PI 3-kinase and PKB [20–23]. However, reduced insulin-stimulated PI 3-kinase activation does not necessarily reduce PKB activation, and insulin was found to promote phosphorylation of PKB normally in insulin-resistant muscles despite a decrease in insulin-stimulated IRS-1-associated PI 3-kinase activity activity [24, 25]. Dexamethasone-induced insulin resistance does not alter tyrosine phosphorylation of the insulin receptor [18, 26], but inhibits insulin-stimulated IRS-1 associated PI 3-kinase activity [26]. The first aim of the present study was to evaluate the role of PKB and GSK-3 in the development of insulin resistance in skeletal muscles during in vivo treatment with dexamethasone.
Pharmacological inhibition of GSK-3 with highly selective, reversible, cell-permeable small molecules can improve insulin sensitivity in insulin-resistant muscles from Zucker diabetic fatty (ZDF) rats [27–29]. A single administration of a GSK-3 inhibitor in ZDF rats improved glucose disposal and increased glycogen synthase activity in liver and muscles [29]. More interestingly, GSK-3 inhibitors increased insulin-stimulated glucose transport in epitrochlearis and soleus muscles from insulin-resistant ZDF rats, but not from insulin-sensitive lean Zucker rats [27, 28]. The enhancement of insulin-stimulated glucose transport response in insulin-resistant muscle may be related to GSK-3’s role in the pathogenesis of insulin resistance, and is probably unrelated to the inhibitor’s effects on glycogen synthase activation [28]. The second aim of the present study was to investigate whether pharmacological inhibition of GSK-3 improves insulin-stimulated glucose uptake and glycogen synthase activation in skeletal muscles from dexamethasone-treated rats.
Materials and methods
Animals
Male Wistar rats (Bk1:Wist; B & K Universal, Nittedal, Norway) were housed at 21°C with a 12:12 h light–dark cycle (light from 07.00 to 19.00 h) and given free access to chow and tap water. Rats were housed individually for 1 week and were divided in two weight-matched groups (280.8±2.9 g for control rats and 282.9±2.8 g for dexamethasone-treated rats, n=28–29). Rats were submitted to a daily intraperitoneal injection of dexamethasone (1.0 mg/kg dissolved in 0.9% NaCl) (Sigma, St Louis, CA, USA) for 12 days. This concentration has previously been reported to induce a state of insulin resistance [16, 26]. Other rats were injected with 0.9% NaCl. In the 18 h preceding the experiment, rats were given 5 g of chow. The experiments were conducted in conformity with the laws and regulations controlling experiments on live animals in Norway and the European Convention for the Protection of Vertebrate Animals used in Experimental and Other Scientific Purposes.
Incubations and tissue removal
Rats were anaesthetised with an intraperitoneal injection of ∼0.5 ml pentobarbital (50 mg/ml). Soleus strips and intact epitrochlearis muscles were dissected out and mounted on apparatus at their approximate resting length and incubated as described previously [30]. Initially, muscles were preincubated for ∼30 min in 3.5 ml Krebs–Henseleit buffer containing 5.5 mmol/l glucose, 2 mmol/l pyruvate, 5 mmol/l HEPES and 0.1% bovine serum albumin, pH 7.4. After preincubation, muscles were incubated for measurement of glucose uptake, glycogen synthesis, or for analysis of insulin signalling as described below. Incubation buffers were continuously gassed at 95% oxygen and 5% carbon dioxide and maintained at 30°C in a water bath. Immediately after incubation, muscles were removed from the apparatus, blotted on filter paper, frozen in liquid nitrogen and stored at −70°C until analysis. After dissection of the soleus and epitrochlearis, the extensor digitorum longus (EDL), heart and liver were rapidly removed, frozen in liquid nitrogen and stored at −70°C until analysis. Finally, epididymal fat pads were removed and weighed.
Glucose uptake
For measurements of glucose uptake, muscles were incubated for 30 min in Krebs–Henseleit buffer containing ∼9.3×106 Bq/l 2-[1,23H(N)]-deoxy-d-glucose (specific activity 1.1×1015 Bq/mol; DuPont-New England Nuclear, Boston, MA, USA) and ∼3.7×106 Bq/l [14C]-mannitol (specific activity 2.1×1012 Bq/mol; DuPont-New England Nuclear) without or with 3 or 60 nmol/l of insulin (Actrapid; Novo Nordisk, Bagsværd, Denmark). Freeze-dried muscle samples were weighed and dissolved in 600 μl of KOH 1 mol/l for 20 min at 70°C. Then 400 μl of the digest was added to 3 ml scintillation solution (Hionic Fluor; Packard Bioscience, Groningen, The Netherlands), mixed, and counted for radioactivity (Tri-Carb 1900 TR; Packard BioScience, Meriden, CT, USA).
Glycogen synthesis
Glycogen synthesis was measured from the incorporation of [14C]-glucose into glycogen. Muscles were incubated for 60 min in Krebs–Henseleit buffer containing ∼7.4×106 Bq/l of d-[14C(U)]-glucose (specific activity 11.2×1012 Bq/mol; DuPont-New England Nuclear) and different insulin concentrations. For analysis of radiolabelled glycogen, muscles were freeze-dried, weighed, and dissolved in 600 μl of KOH 1 mol/l (20 min at ∼70°C). To 500 μl of KOH digest, 100 μl of saturated Na2SO4 and 100 μl glycogen (25 mg/ml) were added and mixed. Cold (∼−70°C) ethanol (1.5 ml) was added and the glycogen was precipitated overnight at −20°C. After centrifugation (3,000 g for 20 min at 4°C) the supernatant was discarded and the precipitate was dissolved in 500 μl of distilled water for 20 min at 70°C, and the glycogen was reprecipitated with addition of cold ethanol (1 ml) and stored for 60 min at −20°C. The new precipitates were dissolved in 300 μl of distilled water and 250 μl of the solution was added to 3 ml of scintillation solution (Hionic Fluor) and counted for radioactivity (Tri-Carb 1900 TR; Packard, USA).
Glycogen concentration
For measurements of glycogen in skeletal muscles, 100 μl of the KOH digest was neutralised with 25 μl acetic acid 7 mol/l prior to addition of 500 μl acetate buffer 0.3 mol/l (pH 4.8) containing 0.2 U/ml of amyloglucosidase (Boehringer–Mannheim, Indianapolis, IN, USA). The glycogen was hydrolysed at 37°C for 3 h and the glucose formed was determined fluorometrically [31]. Glycogen in liver and heart tissues was hydrolysed in 1 mol/l HCl for 2.5 h at 100°C. Because of the high glycogen concentration in the liver, 100 μl of hydrolysate was diluted (1:4) in 1 mol/l HCl. The digests were centrifuged (2,500×g for 10 min at 4°C) and glucose units were measured fluorometrically [31].
Glycogen synthase activity
Glycogen synthase activity was measured in muscles incubated with and without insulin. Glycogen synthase activity was analysed as described before [32]. Glycogen synthase activities were measured without glucose 6-phosphate (G-6-P), with 0.17 mmol/l G-6-P and with 12 mmol/l G-6-P (total activity). The glycogen synthase-independent activity (%) was calculated as the activity of the enzyme in the absence of G-6-P divided by the total activity and multiplied by 100. Glycogen synthase fractional activity (%) was calculated as the activity of the enzyme with 0.17 mmol/l G-6-P divided by the total activity and multiplied by 100.
Plasma glucose
Blood was taken from the vein of the tail between 10.00 and 11.00 h. Blood (20 μl) was added to 500 μl of 0.4 mol/l PCA on ice. For analysis, samples were centrifuged (2,500×g for 10 min at 4°C) and glucose units were measured fluorometrically [31].
Western blot analysis
Skeletal muscles were weighed and homogenised (1 mg w/w, 25 μl) in ice-cold buffer containing 50 mmol/l HEPES, 150 mmol/l NaCl, 10 mmol/l Na4P2O7, 30 mmol/l NaF, 1 mmol/l Na3VO4, 10 mmol/l EDTA, 2.5 mmol/l benzamidine, 0.5 μg/10 mg muscle of protease inhibitor cocktail (Sigma P-8430) and 1% Triton X-100, pH 7.4. Homogenates were rotated for 1 h at 4°C and centrifuged (11,500×g at 4°C for 10 min), as described before [33]. Protein concentration in supernatants was determined by a DC protein assay (Bio-Rad Laboratories, Hercules, CA, USA) according to the instruction manual. Supernatants were diluted to a protein concentration of 3 μg/μl, aliquoted, and stored at −70°C.
For electrophoresis, aliquots were prepared with Laemmli buffer [34], heated at 95°C for 5 min to completely dissociate proteins, and centrifuged at 22 000×g for 15 s. Muscle proteins were separated by electrophoresis in either 8 or 10% SDS–PAGE. Transfer of proteins from the gel onto the polyvinylidene difluoride (PVDF) membrane was performed for 1 h at 200 V in a Mini Trans-Blot cell with a Bio-Ice cooling unit (Bio-Rad Laboratories). The transfer buffer contained 25 mmol/l Tris, 192 mmol/l glycine and 10% methanol. Membranes were washed (3×10 min) in PBS-T (80 mmol/l Na2HPO4, 20 mmol/l NaH2PO4, 100 mmol/l NaCl, 0.1% Tween 20). To avoid non-specific binding of antibody to the PVDF, membranes were blocked in PBS-T containing 5% non-fat milk or 5% BSA (for anti-phosphotyrosine) for 2 h at room temperature. After blocking, membranes were washed in PBS-T (2×30 s), and incubated overnight at 4°C with the primary antibody. After washing in PBS-T (6×10 min), membranes were incubated with the appropriate secondary antibody conjugated to horseradish peroxidase (HRP) for 1 h at room temperature, and washed again (6×10 min). Antibody binding was detected by enhanced chemiluminescence (ECL; Amersham Pharmacia Biotech, Little Chalfont, Buckinghamshire, UK) as described by the manufacturer. Blots were scanned (Scan Jet IIcx; Hewlett Packard, Palo Alto, CA, USA) and signals quantified by densitometry with Scion Image software (Scion Corporation, Frederick, MD, USA).
Antibodies
Anti-phosphotyrosine, anti-PKBα, anti-PKBβ and anti-GSK-3α/β were from Upstate Biotechnology (Lake Placid, NY, USA). Anti-phospho-GSK3α/β (Ser21/Ser9), anti-phospho-PKB (Ser473), anti-phospho-PKB (Thr308) and anti-phospho-p70s6k were from Cell Signalling (Beverly, MA, USA). Anti-phosphoglycogen synthase (Ser645, Ser649, Ser653, Ser657) was from Oncogene (San Diego, CA, USA). p85α was a gift from P. Shepherd (University College London, UK). Antibodies against glycogen synthase and GLUT4 were generous gifts from Oluf Pedersen (Copenhagen, Denmark) and David James (Sydney, Australia), respectively. Anti-rabbit HRP-linked antibody was from New England Biolabs (Beverly, MA, USA). Anti-sheep and anti-mouse HRP-linked antibodies were from Upstate Biotechnology (Lake Placid, NY, USA).
GSK-3 inhibitor
The GSK-3 inhibitor CHIR-637 (also known as CT20026) was obtained from Chiron Corporation (Emeryville, CA, USA). CHIR-637, a low-molecular weight (531 Da) small molecule, is an ATP-competitive inhibitor of GSK-3β giving an IC50 of 4 nmol/l in a cell-free binding assay [35]. This inhibitor is approximately equipotent against both isoforms of GSK-3 (α/β). Like other GSK-3 inhibitors in this class, it exhibits >2,500-fold selectivity against a panel of 16 other protein kinases, including cdc2 and erk2, which are the closest homologues of GSK-3. To the best of our knowledge, CHIR-637 does not interfere with kinases (with the exception of GSK-3) that are involved in the insulin signalling pathway. Demonstrating excellent membrane permeability, glycogen synthase activation was stimulated two- to three-fold above basal in CHIR-637-treated insulin receptor-expressing CHO-IR cells. The concentration of GSK-3 inhibitor causing half-maximal glycogen synthase stimulation (EC50) in CHO-IR cells was 66 nmol/l [35], which is similar to the EC50 observed in soleus muscles in this study (data not shown).
CHIR-637 was diluted in DMSO to obtain a 10 mmol/l stock solution and stored at −20°C. Before experiments, the liquefied stock solution was sonicated and further dissolved in DMSO and added to incubation buffers at the concentration to study. In experiments with CHIR-637, 0.1% DMSO was present in exposed and control muscles. A concentration of 500 nmol/l GSK-3 inhibitor was found to fully activate glycogen synthase in cells (data not shown).
Statistics
Data are presented as means±SEM. Comparisons were initiated by ANOVA. Least significant difference tests were performed post hoc. A value of p<0.05 was considered statistically significant.
Results
Characteristics of rats treated with dexamethasone
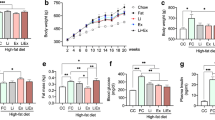
As observed by others, glucocorticoid excess caused slight hyperglycaemia and muscle atrophy (Table 1). Rats treated with dexamethasone had lower body weight and epididymal fat pad weight than control rats (Table 1). After fasting, the glycogen concentration was slightly higher in skeletal muscles of dexamethasone-treated rats than control rats (Table 2). The daily food consumption in control and dexamethasone-treated rats was 23.1±1.8 (n=12) and 15.5±1.0 g (n=8), respectively.
Glucose uptake
In the soleus, insulin-stimulated glucose uptake was lower in dexamethasone-treated rats than in control rats at 3 nmol/l (50%) and 60 nmol/l insulin (38%) (Fig. 1a). In epitrochlearis, dexamethasone inhibited insulin-stimulated glucose uptake by 40% at 3 nmol/l and 25% at 60 nmol/l insulin (Fig. 1b).
Effects of dexamethasone on glucose uptake in skeletal muscles. Muscles from control (open bars) and dexamethasone-treated (filled bars) rats were incubated for 30 min with different concentrations of insulin. a Effect of insulin on glucose uptake in soleus from control and dexamethasone-treated rats. b Effect of insulin on glucose uptake in epitrochlearis from control and dexamethasone-treated rats. dw dry weight. Values are mean±SEM. Number per group: n=7 for soleus; n=10 for epitrochlearis. a p<0.003 vs muscle incubated without insulin from rats exposed to similar treatment; b p<0.01 vs muscle from control rats incubated with a similar insulin concentration; c p<0.002 vs muscle incubated with 3 nmol/l from rats exposed to similar treatment
Glycogen synthesis
Insulin-stimulated glycogen synthesis was decreased in soleus from dexamethasone-treated rats, whereas basal glycogen synthesis was not significantly reduced. Rates of glycogen synthesis were reduced by ∼70% at physiological and supraphysiological insulin concentrations in soleus from dexamethasone-treated rats compared with control rats (Fig. 2a).
Effects of dexamethasone on glycogen synthesis and glycogen synthase activation in soleus muscles. Soleus muscles from control (open bars) and dexamethasone-treated (filled bars) rats were incubated with a tracer amount of 14C glucose for 60 min in the presence of 0, 3 and 60 nmol/l insulin. For glycogen synthase phosphorylation, soleus muscles were incubated for 30 min. Soleus muscles from control rats incubated for 30 min with 60 nmol/l insulin were set at 100% and all values were calculated as a percentage of this. a Effect of insulin on glycogen synthesis in control and dexamethasone-treated rats. b Effect of insulin on glycogen synthase fractional activity in control and dexamethasone-treated rats. c Effect of insulin on glycogen synthase phosphorylation in control and dexamethasone-treated rats. dw dry weight, C control, D dexamethasone-treated GS glycogen synthase pGS glycogen synthase phosphorylation. Values are mean±SEM. n=4–14 for each group. a p<0.04 vs muscle incubated without insulin from rats exposed to similar treatment; b p<0.007 vs muscle from control rats incubated with a similar insulin concentration; c p<0.02 vs muscle incubated with 3 nmol/l from rats exposed to similar treatment
Glycogen synthase activity and glycogen synthase phosphorylation
Insulin increased glycogen synthase fractional activity (Fig. 2b) and glycogen synthase activity in the independent form (data not shown) in soleus from control rats. In muscles from dexamethasone-treated rats, insulin was unable to increase glycogen synthase fractional activity (Fig. 2b) and glycogen synthase activity in the independent form (data not shown). In agreement with these data, insulin decreased glycogen synthase phosphorylation (Ser645, Ser649, Ser653, Ser657) in soleus from control rats, but insulin did not stimulate dephosphorylation of glycogen synthase soleus from dexamethasone-treated rats (Fig. 2c). Glycogen synthase total activity was similar in soleus from control and dexamethasone-treated rats (data not shown).
Effects of dexamethasone on expression of insulin signalling proteins
Expression of glycogen synthase, PKBα, PKBβ, GSK-3α and GSK-3β, as determined by quantification on blots, was similar in control and dexamethasone-treated rats (Fig. 3). Interestingly, expression of the p85α subunit of PI 3-kinase was 30% higher in dexamethasone-treated rats than in control rats (130.0±7.7 and 100.0±3.9% in dexamethasone-treated and control rats, respectively; n=7 in each group, p<0.002). GLUT4 expression was similar in soleus from control and dexamethasone-treated rats. In epitrochlearis, GLUT4 expression was higher in muscles from dexamethasone-treated rats than in control rats (183.7±23.3 vs 100.0±12.3% in dexamethasone-treated and control rats, respectively; n=7 in each group, p<0.0001).
Effects of dexamethasone on expression of insulin signalling protein in soleus muscles. Blots showing expression of different proteins in soleus muscles from control (C) and dexamethasone-treated (D) rats. Expression of the different proteins was quantified by Western blot in muscles from seven control and seven dexamethasone-treated rats
Tyrosine phosphorylation of insulin receptor
Insulin increased tyrosine phosphorylation of the insulin receptor to similar extents in soleus muscles from control and dexamethasone-treated rats (Fig. 4).
Effects of dexamethasone on insulin receptor tyrosine phosphorylation in soleus muscles. Soleus muscles from control (C, open bars) and dexamethasone-treated (D, filled bars) rats were incubated with 0, 3 or 60 nmol/l insulin for 30 min. Soleus muscles from control rats incubated for 30 min with 60 nmol/l insulin were set at 100% and all values were calculated as a percentage of this. IR Insulin receptor, pY tyrosine phosphorylation values are mean±SEM. n=4–6 for each group. a p<0.03 vs muscle incubated without insulin from rats exposed to similar treatment; c p<0.002 vs muscle incubated with 3 nmol/l from rats exposed to similar treatment
PKB phosphorylation
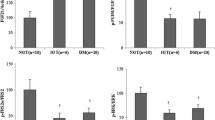
In the basal state, PKB Ser473 phosphorylation was undetectable in control and dexamethasone-treated rats (Fig. 5a). Insulin-stimulated PKB Ser473 phosphorylation was reduced in soleus and epitrochlearis from dexamethasone-treated rats compared with control rats (Fig. 5a,b). PKB Thr308 phosphorylation was investigated at 60 nmol/l insulin and was found to be decreased in soleus muscles from dexamethasone-treated rats (100.0±10.0 and 62.6±5.4% in control and dexamethasone-treated rats, respectively; n=7 in each group, p<0.0001). PKB Thr308 phosphorylation was not detectable in the absence of insulin. Phosphorylation of p70S6K, another PI 3-kinase downstream signalling protein, was reduced at Thr389 by ∼65% in soleus from dexamethasone-treated rats incubated with 60 nmol/l insulin (100.0±22.0 and 34.9±3.9% in control and dexamethasone-treated rats, respectively; n=7 in each group, p<0.0001). Phosphorylation of p70S6K at Thr389 was not detectable in the absence of insulin.
Effects of dexamethasone on PKB phosphorylation in skeletal muscles. Muscles from control (C, open bars) and dexamethasone-treated (D, filled bars) rats were incubated for 30 min with different concentrations of insulin. Muscles from control rats incubated for 30 min with 60 nmol/l insulin were set at 100% and all values were calculated as a percentage of this. a Effect of insulin on PKB phosphorylation in soleus from control and dexamethasone-treated rats. b Effect of insulin on PKB phosphorylation in epitrochlearis from control and dexamethasone-treated rats. Values are mean±SEM. n=7–9 for soleus and n=6–7 for epitrochlearis. a p<0.005 vs muscle incubated without insulin from rats exposed to similar treatment; b p<0.05 vs muscle incubated without CHIR-637 and with a similar insulin concentration; c p<0.0001 vs muscle incubated with 3 nmol/l from rats exposed to similar treatment
Phosphorylation of GSK-3α and GSK-3β
In the basal state, phosphorylation of GSK-3α Ser21 and phosphorylation of GSK-3β Ser9 were similar in soleus from control and dexamethasone-treated rats (Fig. 6a,b). In both groups, insulin increased GSK-3α Ser21 phosphorylation and GSK-3β Ser9 phosphorylation in a dose-dependent manner (Fig. 6a,b). Insulin-stimulated GSK-3α Ser21 and GSK-3β Ser9 phosphorylation were, however, significantly reduced in dexamethasone-treated rats at 3 nmol/l insulin (∼30% for GSK-3α Ser21 phosphorylation and ∼33% for GSK-3β Ser9 phosphorylation) and at 60 nmol/l of insulin (∼23% for GSK-3α Ser21 phosphorylation and ∼26% for GSK-3β Ser9 phosphorylation) (Fig. 6a,b).
Effects of dexamethasone on GSK-3α phosphorylation and GSK-3β phosphorylation in soleus muscles. Soleus muscles from control (C, open bars) and dexamethasone-treated (D, filled bars) rats were incubated with 0, 3 or 60 nmol/l insulin for 30 min. For GSK-3 phosphorylation, soleus from control rats incubated for 30 min with 60 nmol/l insulin were set at 100% and all values were calculated as a percentage of this. a Effect of insulin on GSK-3α phosphorylation in control and dexamethasone-treated rats. b Effect of insulin on GSK-3β phosphorylation in control and dexamethasone-treated rats. Values are mean±SEM. n=11 for each group. a p<0.01 vs muscle incubated without insulin from rats exposed to similar treatment; b p<0.03 vs muscle from control rats incubated with a similar insulin concentration; c p<0.0001 vs. muscle incubated with 3 nmol/l from rats exposed to similar treatment
Effects of CHIR-637 on glycogen synthase activation
CHIR-637 increased glycogen synthase fractional activity in soleus from control and dexamethasone-treated rats (Fig. 7a,b). However, incubation with CHIR-637 did not increase glycogen synthase fractional activity to a similar extent in soleus muscles from dexamethasone-treated and control rats (p<0.05). As expected from the glycogen synthase fractional activity data, CHIR-637 treatment caused dephosphorylation of glycogen synthase in soleus from control and dexamethasone-treated rats (Fig. 7c,d).
Effects of CHIR-637 on glycogen synthase fractional activity and glycogen synthase phosphorylation. Soleus muscles from control (open bars) and dexamethasone-treated (filled bars) rats were preincubated for 60 min without or with (hatched bars) 500 nmol/l CHIR-637. After this incubation, soleus muscles were incubated for an additional 30 min in the presence or absence of 500 nmol/l CHIR-637 and with 0, 3 or 60 nmol/l of insulin. For glycogen synthase phosphorylation, soleus muscles incubated for 30 min with 60 nmol/l insulin and without CHIR-637 were set at 100% and other values were calculated as percentages of this. a Effects of CHIR-637 on glycogen synthase fractional activity in soleus from control rats. b Effects of CHIR-637 on glycogen synthase fractional activity in soleus from dexamethasone-treated rats. c Effects of CHIR-637 on glycogen synthase phosphorylation in soleus from control rats. d Effects of CHIR-637 on glycogen synthase phosphorylation in soleus from dexamethasone-treated rats Values are mean±SEM. n=7–16 for each group. a p<0.02 vs muscle incubated without insulin from rats exposed to similar treatment; b p<0.002 vs. muscle from control rats incubated with a similar insulin concentration; c p<0.02 vs. muscle incubated with 3 nmol/l from rats exposed to similar treatment
Effects of CHIR-637 on insulin-stimulated glucose uptake and PKB phosphorylation
CHIR-637 did not change basal glucose uptake (Fig. 8a,b). More importantly, CHIR-637 did not increase insulin-stimulated glucose uptake (Fig. 8a,b) and PKB phosphorylation (Fig. 8c,d) in soleus muscles from control or dexamethasone-treated rats. In epitrochlearis, pretreatment with CHIR-637 did not increase insulin-stimulated glucose uptake in control or dexamethasone-treated rats (data not shown).
Effects of CHIR-637 on glucose uptake and PKB phosphorylation. Soleus muscles from control (open bars) and dexamethasone-treated (filled bars) rats were preincubated for 60 min without or with (hatched bars) 500 nmol/l CHIR-637. After this incubation, soleus muscles were incubated for an additional 30 min in the presence or absence of 500 nmol/l CHIR-637 and with 0, 3 or 60 nmol/l of insulin. For PKB phosphorylation, soleus muscles incubated for 30 min with 60 nmol/l insulin and without CHIR-637 were set at 100% and other values were calculated as percentages of this. a Effects of CHIR-637 on glucose uptake in soleus from control rats. b Effects of CHIR-637 on glucose uptake in soleus from dexamethasone-treated rats. c Effects of CHIR-637 on PKB phosphorylation in soleus from control rats. d Effects of CHIR-637 on PKB phosphorylation in soleus from dexamethasone-treated rats. dw dry weight. Values are mean±SEM. n=7–11 for each group. a p<0.05 vs muscle incubated without insulin from rats exposed to similar treatment; c p<0.0001 vs muscle incubated with 3 nmol/l from rats exposed to similar treatment
Discussion
Glucocorticoid-induced insulin resistance was confirmed by a 30–50% reduction in insulin-stimulated glucose uptake and a ∼70% reduction in insulin-stimulated glycogen synthesis, in agreement with previous studies [16, 18]. We report that dexamethasone treatment decreases insulin-stimulated PKB and GSK-3 phosphorylation and completely blocks the ability of insulin to dephosphorylate and activate glycogen synthase, without reducing expression of these proteins. Pharmacological inhibition of GSK-3 increased glycogen synthase fractional activity in muscles from dexamethasone-treated rats, but did not improve insulin-stimulated glucose uptake.
Dexamethasone abolished insulin’s ability to increase glycogen synthase fractional activity and to dephosphorylate glycogen synthase at Ser645, Ser649, Ser653, Ser657. GSK-3 phosphorylates these sites, which are the most important for regulation of glycogen synthase activity [11], and insulin reduced glycogen synthase phosphorylation at these sites by ∼50% in soleus from normal rats. The fact that insulin did not dephosphorylate and activate glycogen synthase in muscles from dexamethasone-treated rats shows that glycogen synthesis is more severely affected than glucose uptake. Glycogen content is a strong regulator of glycogen synthase activity [36] and glycogen content was slightly higher in muscles from dexamethasone-treated rats, as expected [19, 37]. The glycogen concentration in muscles from dexamethasone-treated rats was, however, not above the content found in non-fasted rats, in which insulin activates glycogen synthase [38]. High glycogen content, therefore, does not explain the inability to dephosphorylate and activate glycogen synthase activation during insulin stimulation.
In the present study, dexamethasone treatment reduced insulin-stimulated PKB Ser473 and Thr308 phosphorylation by about 50%. In skeletal muscles, PKBβ and PKBα are the two major isoforms. PKBβ seems to regulate insulin-stimulated glucose uptake [12, 13], whereas PKBα seems to regulate muscle growth [39]. The phospho-specific antibodies against PKB Ser473 and PKB Thr308 bind to both isoforms, and it is not possible to separate them on blots. Previous studies have reported reduced PKB activity in diabetic Goto–Kakizaki rats [22] and human subjects with type 2 diabetes mellitus [23]. However, other studies have shown normal PKB phosphorylation in insulin-resistant muscles despite decreased insulin-stimulated IRS-1 associated PI 3-kinase activity [24, 25]. A weakness of the present study is that we have only investigated the effect of a high concentration of dexamethasone on PKB phosphorylation, but our data convincingly show reduced insulin-stimulated PKB phosphorylation in insulin-resistant muscles from dexamethasone-treated rats. Further studies have to confirm whether similar impairments occur in humans during clinical treatment with glucocorticoids.
Insulin-stimulated phosphorylation of GSK-3α and GSK-3β was reduced in muscles from dexamethasone-treated rats. Despite a reduction in insulin-stimulated GSK-3 phosphorylation by about 30% compared with control rats, insulin still elicited a significant increase in GSK-3 phosphorylation in soleus from dexamethasone-treated rats. The fact that insulin-stimulated glycogen synthase activation and dephosphorylation were completely abolished in dexamethasone-treated rats seems, therefore, to be explained only in part by increased GSK-3 activity. We suggest that dexamethasone treatment also impairs activation of protein phosphatase-1, and therefore dephosphorylation of glycogen synthase in response to insulin.
Glucocorticoid receptors regulate DNA transcription, affecting the expression of various proteins. Reduced expression of PKB [40], reduced expression of glycogen synthase [41] or increased expression of GSK-3 [42] causes insulin resistance. In the present study, dexamethasone did not affect expression of PKBα, PKBβ, GSK-3α, GSK-3β or glycogen synthase in skeletal muscles. Expression of GLUT4 has been suggested to determine insulin sensitivity [43], but in agreement with other studies, dexamethasone treatment did not change GLUT4 expression in soleus. In fact, as reported previously [16], glucocorticoid treatment increased GLUT4 expression in the fast-twitch epitrochlearis muscles, probably reflecting the fact that fast-twitch muscles atrophy more than slow-twitch muscles, resulting in higher relative content of membrane proteins. Our data therefore suggest that dexamethasone induces skeletal muscle insulin resistance by impairing phosphorylation of insulin signalling proteins rather than reducing expression of GLUT4, PKB, GSK-3 or glycogen synthase.
Dexamethasone induces insulin resistance in skeletal muscle without reducing tyrosine phosphorylation of insulin receptor. Insulin-stimulated tyrosine phosphorylation of IRS-1 has also been reported to be normal, whereas dexamethasone treatment reduces IRS-1-associated PI 3-kinase activity [26]. PI 3-kinase is a heterodimer composed of a regulatory subunit (p85α) and a catalytic subunit (p110), and PI 3-kinase is activated when the dimer binds to IRS-1 [9]. It has been hypothesised that p85α exists as a free monomer or bound to p110 [44]. Binding of free p85α monomer to IRS-1 does not increase PI 3-kinase activity, but instead competes with binding of the p85α-p110 heterodimer, and consequently impairs PI 3-kinase activation [44]. Support for this hypothesis comes from studies showing that overexpression of p85α reduces insulin signalling in L6 myotubes [45], whereas reduced p85α expression improves glucose homeostasis and insulin signalling in normal and insulin-resistant mice [46, 47]. Our data support the possibility that increased expression of p85α and competitive inhibition of PI 3-kinase activity may mediate glucocorticoid-induced insulin resistance.
It has been suggested that GSK-3 inhibitors represent a potential therapeutic treatment for type 2 diabetic patients [35]. In the present study, we found that the GSK-3 inhibitor CHIR-637 increased glycogen synthase fractional activity in soleus from normal and dexamethasone-treated rats. This finding is consistent with previous reports showing that GSK-3 inhibitors activate glycogen synthase in lean and ZDF rats [27], and in cultured human skeletal muscle cells from normal and type 2 diabetics [48]. In the present study, CHIR-637 was unable to restore glycogen synthase activation in muscle from dexamethasone-treated rats to that found in muscles from normal rats. While it is difficult to accurately gauge the percentage of GSK-3 which was inhibited in these experiments, the incomplete and slow dephosphorylation of glycogen synthase suggests a lack of protein phosphatase-1 activity in dexamethasone-treated rat muscle. However, the fact that insulin-stimulated glycogen synthase activation was completely blocked in muscles from dexamethasone-treated rats highlights the potential of GSK-3 inhibitors in the treatment of type 2 diabetes mellitus. It is noteworthy that the specific effect of CHIR-637 is supported by reduced glycogen synthase phosphorylation at sites phosphorylated by GSK-3.
Short-term incubation with CHIR-637 did not increase insulin-stimulated glucose uptake or PKB phosphorylation in muscles from dexamethasone-treated rats. Pharmacological inhibition of GSK-3 increases insulin-stimulated glucose uptake in insulin-resistant skeletal muscles from obese ZDF rats but not in muscle from insulin-sensitive lean ZDF rats [27, 28]. It is not expected that GSK-3 inhibition would have a direct effect on PKB phosphorylation, but GSK-3 has been reported to phosphorylate IRS-1, which reduces activation of PI 3-kinase and PKB [49]. While dexamethasone-induced diabetes in rats may share some of the traits of ZDF rats, insulin-stimulated glucose uptake and PKB phosphorylation were not increased by GSK-3 inhibition in muscles from dexamethasone-treated rats. Inhibition of GSK-3 by CHIR-637 may increase glucose transport in ZDF rats by reducing IRS-1 serine phosphorylation, but there is no evidence that dexamethasone increases serine phosphorylation of IRS-1. In human skeletal muscle cells, however, this class of GSK-3 inhibitor only enhanced insulin-stimulated glucose uptake after prolonged (>6 h) exposure [48]. It is therefore possible that prolonged incubation of muscle from dexamethasone-treated rats with CHIR-637 might result in increased glucose transport. Further experiments are required to determine whether chronic treatment with GSK-3 inhibitors will increase insulin sensitivity in dexamethasone-induced insulin-resistant muscles.
In conclusion, dexamethasone treatment impairs insulin-stimulated glucose uptake and glycogen synthesis in muscle, and our data suggest that insulin resistance may result from increased expression of the p85α subunit of PI 3-kinase and reduced PKB phosphorylation. Reduced GSK-3 phosphorylation may contribute to, but not fully explain, the ability of insulin to activate glycogen synthase. Short-term pharmacological inhibition of GSK-3 increased glycogen synthase fractional activity in muscles from dexamethasone-treated rats but did not improve insulin-stimulated glucose uptake.
Abbreviations
- EDL:
-
extensor digitorum longus
- G-6-P:
-
glucose 6-phosphate
- GSK-3:
-
glycogen synthase kinase-3
- PI 3-kinase:
-
phosphatidylinositol 3-kinase
- PKB:
-
protein kinase B
- ZDF:
-
Zucker diabetic fatty rat
References
Nosadini R, Del Prato S, Tiengo A et al (1983) Insulin resistance in Cushing’s syndrome. J Clin Endocrinol Metab 57:529–536
Quddusi S, Browne P, Toivola B et al (1998) Cushing syndrome due to surreptitious glucocorticoid administration. Arch Intern Med 158:294–296
Pagano G, Cavallo-Perin P, Cassader M et al (1983) An in vivo and in vitro study of the mechanism of prednisone-induced insulin resistance in healthy subjects. J Clin Invest 72:1814–1820
Rosmond R (2003) Stress induced disturbances of the HPA axis: a pathway to Type 2 diabetes? Med Sci Monit 9:RA35–RA39
Kusunoki M, Cooney GJ, Hara T et al (1995) Amelioration of high-fat feeding-induced insulin resistance in skeletal muscle with the antiglucocorticoid RU486. Diabetes 44:718–720
Buckbinder L, Robinson RP (2002) The glucocorticoid receptor: molecular mechanism and new therapeutic opportunities. Curr Drug Targets Inflamm Allergy 1:127–136
Gower WR Jr (1993) Mechanism of glucocorticoid action. J Fla Med Assoc 80:697–700
Bryant NJ, Govers R, James DE (2002) Regulated transport of the glucose transporter GLUT4. Nat Rev Mol Cell Biol 3:267–277
Shepherd PR, Withers DJ, Siddle K (1998) Phosphoinositide 3-kinase: the key switch mechanism in insulin signalling. Biochem J 333:471–490
Cross DA, Alessi DR, Cohen P et al (1995) Inhibition of glycogen synthase kinase-3 by insulin mediated by protein kinase B. Nature 378:785–789
Lawrence JC Jr, Roach PJ (1997) New insights into the role and mechanism of glycogen synthase activation by insulin. Diabetes 46:541–547
Jiang ZY, Zhou QL, Coleman KA et al (2003) Insulin signaling through Akt/protein kinase B analyzed by small interfering RNA-mediated gene silencing. Proc Natl Acad Sci U S A 100:7569–7574
Katome T, Obata T, Matsushima R et al (2003) Use of RNA interference-mediated gene silencing and adenoviral overexpression to elucidate the roles of AKT/protein kinase B isoforms in insulin actions. J Biol Chem 278:28312–28323
DeFronzo RA, Gunnarsson R, Bjorkman O et al (1985) Effects of insulin on peripheral and splanchnic glucose metabolism in noninsulin-dependent (type II) diabetes mellitus. J Clin Invest 76:149–155
Shulman GI, Rothman DL, Jue T et al (1990) Quantitation of muscle glycogen synthesis in normal subjects and subjects with non-insulin-dependent diabetes by 13C nuclear magnetic resonance spectroscopy. N Engl J Med 322:223–228
Haber RS, Weinstein SP (1992) Role of glucose transporters in glucocorticoid-induced insulin resistance. GLUT4 isoform in rat skeletal muscle is not decreased by dexamethasone. Diabetes 41:728–735
Dimitriadis G, Leighton B, Parry-Billings M et al (1997) Effects of glucocorticoid excess on the sensitivity of glucose transport and metabolism to insulin in rat skeletal muscle. Biochem J 321:707–712
Leighton B, Challiss RA, Lozeman FJ et al (1987) Effects of dexamethasone treatment on insulin-stimulated rates of glycolysis and glycogen synthesis in isolated incubated skeletal muscles of the rat. Biochem J 246:551–554
Coderre L, Srivastava AK, Chiasson JL (1992) Effect of hypercorticism on regulation of skeletal muscle glycogen metabolism by insulin. Am J Physiol Endocrinol Metab 262:E427–E433
Björnholm M, Kawano Y, Lehtihet M et al (1997) Insulin receptor substrate-1 phosphorylation and phosphatidylinositol 3-kinase activity in skeletal muscle from NIDDM subjects after in vivo insulin stimulation. Diabetes 46:524–527
Goodyear LJ, Giorgino F, Sherman LA et al (1995) Insulin receptor phosphorylation, insulin receptor substrate-1 phosphorylation, and phosphatidylinositol 3-kinase activity are decreased in intact skeletal muscle strips from obese subjects. J Clin Invest 95:2195–2204
Krook A, Kawano Y, Song XM et al (1997) Improved glucose tolerance restores insulin-stimulated Akt kinase activity and glucose transport in skeletal muscle from diabetic Goto–Kakizaki rats. Diabetes 46:2110–2114
Krook A, Roth RA, Jiang XJ et al (1998) Insulin-stimulated Akt kinase activity is reduced in skeletal muscle from NIDDM subjects. Diabetes 47:1281–1286
Kruszynska YT, Worrall DS, Ofrecio J et al (2002) Fatty acid-induced insulin resistance: decreased muscle PI3K activation but unchanged Akt phosphorylation. J Clin Endocrinol Metab 87:226–234
Nadler ST, Stoehr JP, Rabaglia ME et al (2001) Normal Akt/PKB with reduced PI3K activation in insulin-resistant mice. Am J Physiol Endocrinol Metab 281:E1249–E1254
Saad MJ, Folli F, Kahn JA et al (1993) Modulation of insulin receptor, insulin receptor substrate-1, and phosphatidylinositol 3-kinase in liver and muscle of dexamethasone-treated rats. J Clin Invest 92:2065–2072
Henriksen EJ, Kinnick TR, Teachey MK et al (2003) Modulation of muscle insulin resistance by selective inhibition of GSK-3 in Zucker diabetic fatty rats. Am J Physiol Endocrinol Metab 284:E892–E900
Ring DB, Johnson KW, Henriksen EJ et al (2003) Selective glycogen synthase kinase 3 inhibitors potentiate insulin activation of glucose transport and utilization in vitro and in vivo. Diabetes 52:588–595
Cline GW, Johnson K, Regittnig W et al (2002) Effects of a novel glycogen synthase kinase-3 inhibitor on insulin-stimulated glucose metabolism in Zucker diabetic fatty (fa/fa) rats. Diabetes 51:2903–2910
Aslesen R, Jensen J (1998) Effects of epinephrine on glucose metabolism in contracting rat skeletal muscles. Am J Physiol Endocrinol Metab 275:E448–E456
Lowry OH, Passonneau JV (1972) A flexible system of enzymatic analysis, 1st edn. Academic, New York
Franch J, Aslesen R, Jensen J (1999) Regulation of glycogen synthesis in rat skeletal muscle after glycogen-depleting contractile activity: effects of adrenaline on glycogen synthesis and activation of glycogen synthase and glycogen phosphorylase. Biochem J 344:231–235
Whitehead JP, Soos MA, Aslesen R et al (2000) Contraction inhibits insulin-stimulated insulin receptor substrate-1/2-associated phosphoinositide 3-kinase activity, but not protein kinase B activation or glucose uptake, in rat muscle. Biochem J 349:775–781
Laemmli UK (1970) Cleavage of structural proteins during the assembly of the head of bacteriophage T4. Nature 227:680–685
Wagman AS, Johnson KW, Bussiere DE (2004) Discovery and development of GSK3 inhibitors for the treatment of type 2 diabetes. Curr Pharm Des 10:1105–1137
Danforth W (1965) Glycogen synthetase activity in skeletal muscle. Interconversion of two forms and control of glycogen synthesis. J Biol Chem 240:588–593
Coderre L, Srivastava AK, Chiasson JL (1992) Effect of hypercorticism on regulation of skeletal muscle glycogen metabolism by epinephrine. Am J Physiol Endocrinol Metab 262:E434–E439
Jensen J, Aslesen R, Jebens E et al (1999) Adrenaline-mediated glycogen phosphorylase activation is enhanced in rat soleus muscle with increased glycogen content. Biochim Biophys Acta 1472:215–221
Glass DJ (2003) Signalling pathways that mediate skeletal muscle hypertrophy and atrophy. Nat Cell Biol 5:87–90
Garofalo RS, Orena SJ, Rafidi K et al (2003) Severe diabetes, age-dependent loss of adipose tissue, and mild growth deficiency in mice lacking Akt2/PKB beta. J Clin Invest 112:197–208
Park KS, Ciaraldi TP, Carter L et al (2000) Induction of insulin resistance in human skeletal muscle cells by downregulation of glycogen synthase protein expression. Metabolism 49:962–968
Nikoulina SE, Ciaraldi TP, Mudaliar S et al (2000) Potential role of glycogen synthase kinase-3 in skeletal muscle insulin resistance of type 2 diabetes. Diabetes 49:263–271
Ivy JL (2004) Muscle insulin resistance amended with exercise training: role of GLUT4 expression. Med Sci Sports Exerc 36:1207–1211
Giorgino F, Pedrini MT, Matera L et al (1997) Specific increase in p85alpha expression in response to dexamethasone is associated with inhibition of insulin-like growth factor-I stimulated phosphatidylinositol 3-kinase activity in cultured muscle cells. J Biol Chem 272:7455–7463
Ueki K, Algenstaedt P, Mauvais-Jarvis F et al (2000) Positive and negative regulation of phosphoinositide 3-kinase-dependent signaling pathways by three different gene products of the p85alpha regulatory subunit. Mol Cell Biol 20:8035–8046
Mauvais-Jarvis F, Ueki K, Fruman DA et al (2002) Reduced expression of the murine p85alpha subunit of phosphoinositide 3-kinase improves insulin signaling and ameliorates diabetes. J Clin Invest 109:141–149
Terauchi Y, Tsuji Y, Satoh S et al (1999) Increased insulin sensitivity and hypoglycaemia in mice lacking the p85 alpha subunit of phosphoinositide 3-kinase. Nat Genet 21:230–235
Nikoulina SE, Ciaraldi TP, Mudaliar S et al (2002) Inhibition of glycogen synthase kinase 3 improves insulin action and glucose metabolism in human skeletal muscle. Diabetes 51:2190–2198
Eldar-Finkelman H, Krebs EG (1997) Phosphorylation of insulin receptor substrate 1 by glycogen synthase kinase 3 impairs insulin action. Proc Natl Acad Sci U S A 94:9660–9664
Acknowledgements
We thank Jorid Thrane Stuenæs, Ada Ingvaldsend and Astrid Bolling for assistance in some of the experiments, and Einar Eilertsen, Frøydis Kristoffersen and Synøve Bro for animal care. The study was supported by the Research Council of Norway, Novo Nordisk Foundation, and Aktieselskabet Freia Chocolade Fabriks Medisinske Fond.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ruzzin, J., Wagman, A.S. & Jensen, J. Glucocorticoid-induced insulin resistance in skeletal muscles: defects in insulin signalling and the effects of a selective glycogen synthase kinase-3 inhibitor. Diabetologia 48, 2119–2130 (2005). https://doi.org/10.1007/s00125-005-1886-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-005-1886-0